There’s a hidden link between fat in your liver and stubborn high blood sugar that many people, even those at a normal weight, miss. This post shows how excess liver fat makes your body stop responding to insulin, why cutting sugar alone often fails, and practical steps you can use to lower liver fat, improve blood sugar, and regain control of your health.
We will go deeper into the relationship between liver and diabetes type 2.
Key Takeaways:
- A fatty liver— sometimes called hepatic steatosis — often drives insulin resistance and Type 2 diabetes disease — it can happen even if you look thin.
- Lowering liver fat quickly improves blood sugar — fasting or cutting carbs lets the liver burn stored fat, helping insulin work better.
- Start simple: try time‑restricted eating (like 16:8), cut sugary drinks and processed carbs, and eat liver‑friendly foods (eggs, broccoli, kale).
Understanding Fatty Liver
Your liver quietly controls how your body stores and releases energy, and when it fills with fat it stops accepting glucose efficiently. You can be thin and still have a fatty liver (TOFI); excess refined carbs and fructose drive de novo lipogenesis, packing fat into liver cells so they stop clearing sugar. Clinically, this explains why cutting table sugar alone often fails to lower your fasting glucose—the liver is the bottleneck.
The Role of Insulin and the Twin Cycle
Insulin tells cells to take up glucose, but when you eat often or rely on refined carbs, insulin stays high and signals the liver to store energy as fat. That persistent insulin prevents the liver from burning stored fat, so hepatic insulin resistance grows. Lowering insulin—By implementing a healthy diet for fatty liver and type 2 diabetes disease, you let the liver start mobilizing that stored fat and improve blood sugar control.
The Twin Cycle Hypothesis links two vicious loops: excess liver fat impairs insulin control and spills fat into the pancreas, damaging beta-cell function. You get rising blood sugar and higher insulin levels, which feed more liver fat. Studies show that reducing liver fat first improves insulin sensitivity and can stop the pancreatic spillover that worsens diabetes.
Practical evidence supports this: the DiRECT trial used a low-calorie total diet replacement (~800 kcal/day) and achieved diabetes remission in about 46% of participants at 1 year, driven by rapid liver fat loss and weight loss. In other controlled metabolic studies, liver fat and fasting glucose improved within days to weeks of strict calorie or carb restriction, showing the Twin Cycle can be interrupted quickly when you target the liver.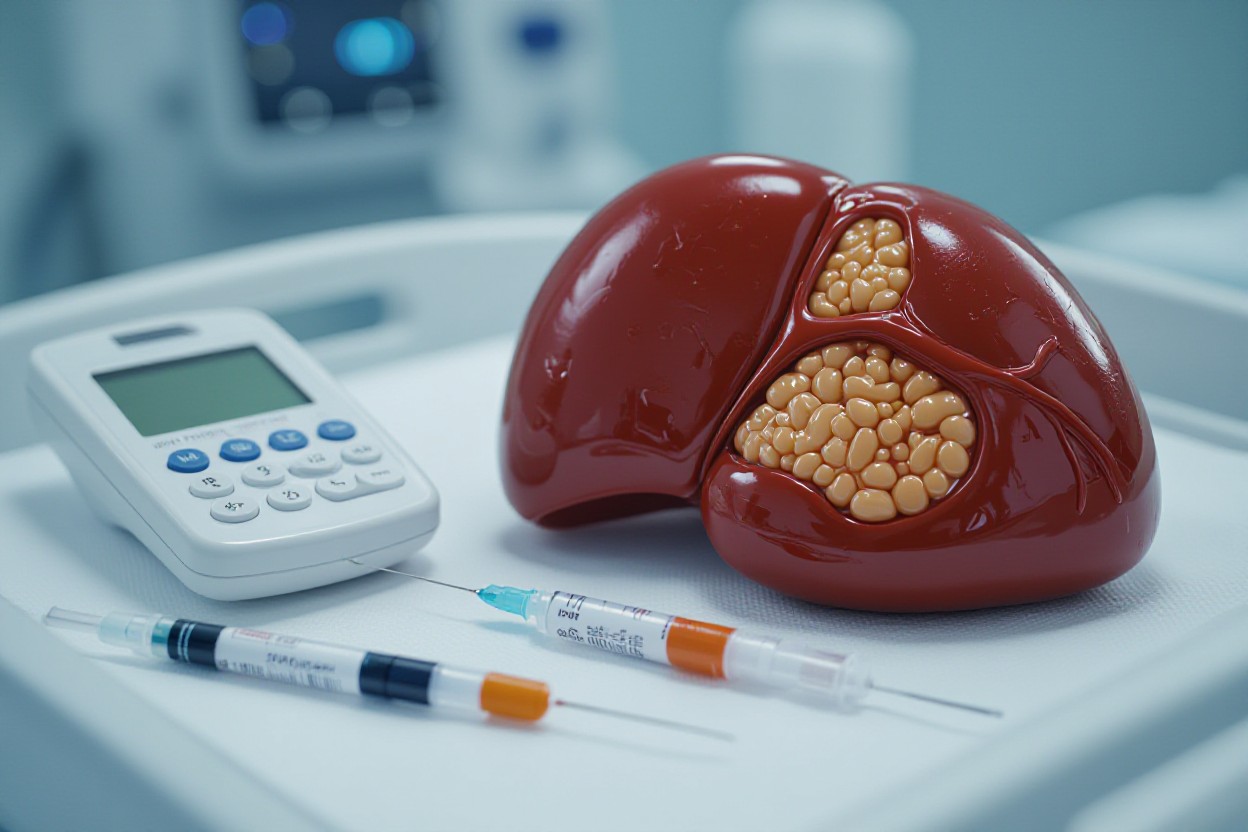
Fatty Liver and Diabetes Relation
When your liver fills with fat, it can become less responsive to insulin, which means it might keep releasing glucose into your blood even if you haven’t eaten. The good news is that clinical studies show that liver fat can decrease surprisingly quickly — often within just 2 to 3 weeks of following a low-carb or fasting plan. In fact, fasting glucose levels may return to normal within about a week in some studies.
To maintain long-term blood sugar health, it’s crucial to tackle the root liver problem causing the issue.
Eating too many carbs and fructose can tell your liver to make and store fat, which can mess with how insulin works. When that happens, your liver and muscles don’t soak up glucose as they should. To make up for it, your pancreas produces more insulin, keeping your insulin levels high over time. This can make it tougher to burn off liver fat, leaving your blood sugar levels high even if you cut out table sugar.
The Twin Cycle helps explain how fat from the liver can overflow into the pancreas, affecting beta‑cells and increasing insulin requirements. Research by Roy Taylor and others shows that when you significantly cut down on liver fat—using methods like very low‑calorie diets or time‑restricted eating—the liver’s insulin sensitivity can improve in just days.
At the same time, the pancreas begins to recover, breaking the cycle before you’ve lost a lot of weight. In practical terms, it’s helpful to lower insulin levels first, which allows the liver to release and burn stored fat more easily.
Effective quick-start strategies include following a 16:8 fasting schedule, reducing intake of fructose and refined carbs, and temporarily cutting calories (clinical studies have used about 800 kcal per day). It’s a good idea to keep track of your fasting glucose and liver health markers; many people notice meaningful reductions in glucose within a few weeks, with ongoing metabolic improvements over 3 to 6 months.
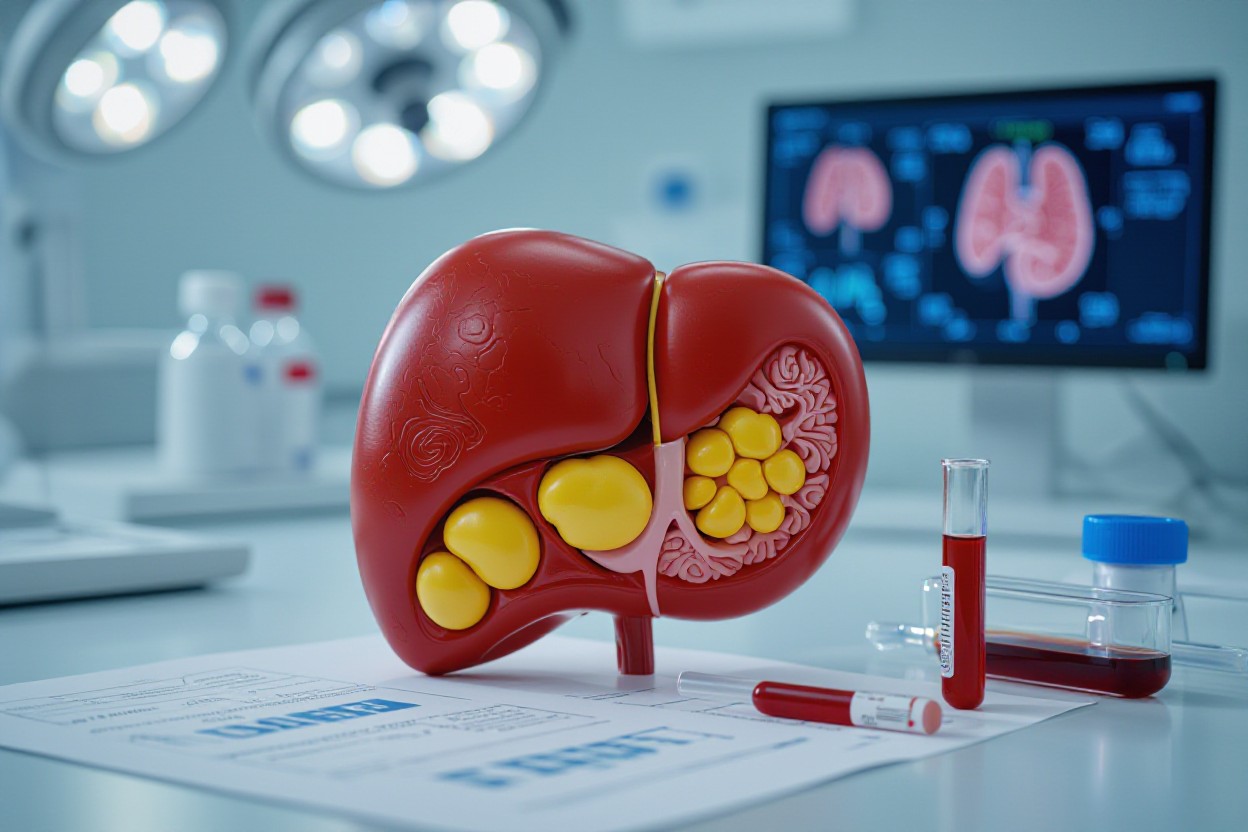
Treatment Perspectives
Did you know that about 25–30% of adults have excess fat in their liver? That fat can increase insulin resistance by causing the liver to release glucose when it shouldn’t. Even if your BMI is normal, you can still be TOFI, so maintaining a normal weight doesn’t mean you’re entirely in the clear. It’s a good idea to get an ultrasound or a FibroScan and keep an eye on your ALT/AST levels. Early signs of liver fat often appear before any symptoms show, and by taking care of your liver, you can help lower your fasting glucose levels and ease the workload on your pancreas.
Try combining simple lifestyle changes like starting with a 16:8 fasting schedule, then exploring low-carb or Healthy Keto diets. Incorporate choline-rich foods such as eggs and liver, eat plenty of vegetables, stay well-hydrated, and avoid processed seed oils. Many people notice reduced liver fat within just 2–3 weeks and enjoy more apparent metabolic benefits over 3–6 months.
Begin with the Metabolic Pause (16:8) and gradually try occasional 24-hour fasts if it feels comfortable. Keep carbs low initially—many find under 50 grams per day is effective for reducing insulin spikes. Consider adding evidence-based supplements, such as omega‑3s, appropriate vitamin D, and herbal options like milk thistle and bitter greens, with your healthcare provider’s guidance. Regularly check your fasting glucose and A1c, and consider repeating imaging tests to see your liver fat decrease and fine-tune your plan as your insulin sensitivity improves.

Fatty liver diabetes type 2 treatment
Begin with a simple, step-by-step plan: try a Metabolic Pause (16:8 TRE), reduce fructose and refined carbs, replace seed oils with olive or avocado oil, and include liver-friendly foods like eggs (rich in choline), broccoli (full of sulforaphane), and fatty fish (high in omega-3s). You should see noticeable liver-fat reduction in just 2–3 weeks, with ongoing metabolic improvements over 3–6 months when you combine fasting, balanced eating, good sleep, and regular activity.
Begin with 12:12 for a week, move to 16:8 (standard: noon–8 pm), and progress to 18:6 if it fits your lifestyle. Fasting lowers insulin levels and depletes liver glycogen after about 12–16 hours, allowing your liver to burn stored fat. Use water, black coffee, or herbal tea during fasts, and stop if you’re on insulin or other meds without medical guidance.
Remove sugary drinks, fruit juices, and processed carbs; cut high-fructose corn syrup and most sweets. Add choline-rich eggs (one large egg ≈, 147 mg choline), daily servings of cruciferous vegetables, oily fish twice weekly, and fiber-rich vegetables to help export liver fat. Swap seed oils for extra-virgin olive or avocado oil to reduce inflammation.
Practical meal examples: breakfast—2-egg omelet with broccoli and spinach; lunch—salmon salad with avocado and mixed greens; snack—handful of walnuts or a small serving of berries; dinner—roasted chicken with kale and cauliflower. Aim for 1–2 cruciferous servings per day, ~25–30 g fiber daily, and one egg daily for choline; these choices help your liver package and remove fat while stabilizing blood sugar.
Frequently Asked Questions
Reversal of Fatty Liver and Diabetes
Yes — you can reverse both. Clinical studies show liver fat can drop 30–50% within 2–3 weeks of strict carb restriction or fasting, and many patients see fasting glucose and A1c improve within weeks. When you lower insulin with a Metabolic Pause and low‑carb plan, the liver starts to burn stored fat and the pancreas often recovers, so your blood sugars fall without simply adding more medications.
Normal Weight and hepatic steatosis
Being a normal weight doesn’t protect you. Up to about 20% of lean adults have excess liver fat (TOFI), often from past high‑carb diets, fructose intake, or genetics. You may wear a small clothing size but still have a hepatic steatosis that keeps dumping glucose into your blood, which is why cutting table sugar alone often doesn’t fix high fasting glucose.
Look for subtle signs: normal ALT/AST can be misleading because enzymes rise late. If you have stubborn fasting glucose, high fasting insulin, or a triglyceride/HDL ratio above ~3, ask for imaging (ultrasound, FibroScan, or MRI‑PDFF) to check liver fat. Simple steps—time‑restricted eating, cutting refined carbs and fructose, and adding choline foods—often shrink liver fat and improve your numbers within weeks.
Clinical Insights and Expert Opinions
Leading clinicians like Roy Taylor, Jason Fung, and Eric Berg point squarely at liver fat as the trigger, and you should heed their practical guidance: Taylor’s twin‑cycle work and a Diabetologia study show insulin sensitivity can normalize within days after reducing liver fat; Fung recommends intermittent fasting (16:8 or longer) to lower insulin and drain liver stores; Berg warns that high carbs and fructose — not dietary fat — drive liver fat, so cut liquid sugars and refined carbs first.
You may believe diabetes is only a pancreas problem or that only overweight people get hepatic steatosis. In reality, TOFI (thin outside, fat inside) is common, and metabolic damage shows up long before liver enzymes rise. Simply removing table sugar often fails because frequent carbs and high insulin keep liver fat stored; your goal must be to lower insulin, not just sugar intake.
Many also think eating fat causes fatty liver, but studies and clinical cases show excess carbs and fructose force the liver to turn sugar into fat. You should know that regular AST/ALT tests don’t guarantee a healthy liver — fatty buildup can be present despite normal enzyme levels. Acting early with time‑restricted eating, removing fructose, and adding choline‑rich foods can drop liver fat in 2–3 weeks and improve your glucose before you lose weight.
Conclusion
With these considerations, you should understand that fatty liver often lies behind stubborn high blood sugar, and by treating your liver with targeted fasting, lower carbs, and better food choices you can help insulin work better and lower your diabetes risk. New findings on gut signals add depth to this view — see Surprising gut discovery reveals a hidden trigger of … for more on how body systems connect to your liver and blood sugar.
FAQ
Q: Why do some people with a normal weight develop Type 2 Diabetes?
A: Even if you look slim on the outside, you can carry fat inside your organs, especially the liver and pancreas. That hidden fat makes the liver stop taking up glucose properly and forces the pancreas to work harder. Over time the body stops responding well to insulin (the hormone that moves sugar into cells), and blood sugar rises. This can happen from eating lots of refined carbs or fructose, frequent snacking, genetics, low activity, or long periods without giving the body a break from eating.
Q: I cut out sugar but my blood sugar stays high — why?
A: Cutting table sugar helps, but the liver can still make fat from other carbs (breads, rice, fruit sugars) and keep driving high blood sugar. If your liver is full of fat, it keeps sending glucose into the blood and keeps insulin high, even if you stopped eating sweets. To lower blood sugar you need to lower insulin so the liver can burn its fat — practical steps are time‑restricted eating (like 16:8), cutting back on starchy and processed carbs, removing sugary drinks and high‑fructose foods, and focusing on whole foods that support the liver.
Q: Can fatty liver and Type 2 Diabetes be reversed, and how long does it take?
A: Yes — the liver can heal and many people see big drops in blood sugar within weeks when they lower liver fat. Studies and clinical experience show liver fat can fall in 2–3 weeks with strict carb reduction or fasting, and fuller metabolic recovery often happens over 3–6 months of steady changes. Key steps: use time‑restricted eating or intermittent fasting to lower insulin, avoid liquid sugars and processed carbs, eat liver‑helping foods (eggs, cruciferous vegetables), stay active, and work with your healthcare provider to adjust medicines and monitor progress.

